Memorial Health System Rehabilitation and Sports Medicine provides friendly, caring, and quality services to restore individuals to their highest level of functioning to help them get back to doing what they love. Located at Memorial Hospital in Abilene, Kansas, MHS Rehabilitation and Sports Medicine offers physical therapy, occupational therapy, speech therapy, recovery care, ASTYM, sports medicine, and concussion management services. Services are available with or without a physician’s referral. Please call us at (785) 263-6664 if you need more information.


Physical Therapy
MHS Rehabilitation and Sports Medicine wants to help you get back to doing what you love most. We have a specially trained physical therapy staff to assist with improving each patient’s movement potential through the use of:
- Heat, ice, massage, and electrical stimulation to bring about therapeutic effects
- Exercise to strengthen or re-educate muscles to enhance joint motion
- Exercise for general conditioning or cardiopulmonary reconditioning
- Balance and gait training
- Aquatic therapy
- ASTYM (Augmented Soft Tissue Mobilization)
- Orthopedic rehabilitation following total joint replacements
- Manual therapy, deep tissue, and soft tissue mobilization
- Post surgical rehabilitation
- Back and neck pain treatment and education
Occupational Therapy
The goal of MHS Rehabilitation and Sports Medicine’s occupational therapy services is to increase overall independence with daily tasks.
Services include:
- Orthosis fitting and training
- Adaptive device and compensatory techniques training
- Wheelchair positioning and adaptation
- Activities of daily living training
- Assessment to ensure safety and efficiency at home and work
- Disability analysis
- Hand therapy
- Sensory integration
- Various modalities
What can Occupational Therapy do for you?
Speech Therapy
MHS Rehabilitation and Sports Medicine’s speech-language therapy helps those with communication, speech, language, and swallowing disorders. Services are available from newborns to elderly.
- Aphasia evaluation/therapy
- Cognitive evaluation/therapy
- Dysarthria evaluation/therapy
- Swallowing evaluation/therapy
- Articulation therapy
- Fluency training
- Phonological assessment/therapy
- Assistive and augmentative communication devices
- Voice therapy
- Modified barium swallow

ASTYM
ASTYM, which stands for Augmented Soft Tissue Mobilization, is a non-invasive therapy that treats soft tissue injuries through the use of patented instruments. The ASTYM treatment has been shown to be effective treating damaged soft tissue resulting from injury, surgery, or other stresses. It also helps eliminate scar tissue problems and rejuvenate muscles, tendons, and ligaments.
Dry Needling
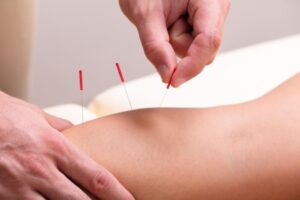 Dry needling is a newer approach in Western Medicine. Although the tools and procedure are very similar to acupuncture, physical therapists that use dry needling are most often using it within their treatment plan; incorporating it with other interventions to treat the patient.
Dry needling is a newer approach in Western Medicine. Although the tools and procedure are very similar to acupuncture, physical therapists that use dry needling are most often using it within their treatment plan; incorporating it with other interventions to treat the patient.
In dry needling procedures, fine needles are inserted just into the skins surface. These particular needles do not inject any fluid into the body, thus the word dry. Dry needling procedures are often used by those who suffer from sports injuries, common muscle aches and pain, arthritis, or even fibromyalgia pain. By easing muscular pain and stiffness a person may regain their range of flexibility and motion.
For more information or to schedule an appointment with Kyle Bowers, please call Rehabilitation and Sports Medicine at (785) 263-6664

Orthopedics
Dr. Todd Herrenbruck and Dr. Todd Reilly are both orthopedic doctors who visit Abilene on different days of the month to offer an orthopedic clinic at Memorial Health System Rehabilitation and Sports Medicine. Please look under our Providers section of our website to find information on visiting specialists; including contact information, and the locations where they hold their clinics.
Sports Medicine
This specialized therapy is offered at the MHS Rehabilitation Services and Sports Medicine office and local schools for athletes.
It involves not only the treatment of sports-related injuries, but preventive education for safe participation in competitive sports, fitness, or recreational activities. The sports medicine program offers concussion management services, providing baseline screenings for student athletes prior to the beginning of the season to use as comparative data in case the athlete has a concussion.
Data is compared with the ImPACT test, performed post-concussion, so the physician may make an informed return-to-play decision.
- Summer Athletic Training
Studies show that female athletes have 4-6 times increased risk for ACL injury compared to males participating at the same level in similar sports. The data show that females jump differently than males.
Memorial Health System’s Sports Medicine Program offers a summer training session for female athletes in grades 7 through 10. The session is designed to help student athletes prevent injury and improve performance by providing training in strengthening, jumping, flexibility, and dynamic warm-up. The primary purpose of the program is to help prevent knee injuries.
The training typically begins in late June and is held at Impact Sports and Fitness, 418 N. Broadway. Registration is due a week before training begins. Interested individuals may contact Memorial Health System Rehabilitation and Sports Medicine at (785) 263-6664.
- Youth Sports Medicine Programs
Memorial Health System Rehabilitation and Sports Medicine makes youth sports medicine programs available to area schools. Our Athletic Trainer treats sports-related injuries and provides preventative education for safe participation in competitive sports, fitness, or recreational activities. For the safety and well-being of youth, our athletic trainer is also readily available at local school youth sporting events to assist athletes.
MHS Rehabilitation and Sports Medicine recognizes the dangers of concussions in sports, particularly for young athletes whose brains can suffer long-term consequences from concussions if not treated properly. That’s why we offer concussion management services. We provide baseline screenings for student athletes prior to the beginning of the season to use as comparative data in case the athlete has a concussion. Objective data helps the athlete’s physician make an informed return-to-play decision.
Baseline screenings for concussions are offered onsite free of charge to students served by youth sports medicine programs.
- Concussion Management
A concussion is a brain injury. Concussions are caused by a bump, blow, or jolt to the head or body. Even what seems to be a mild bump or blow to the head can be serious.
Student athlete concussions are a serious issue, and Memorial Health System’s Sports Medicine Program urges parents of students and students playing contact sports to take concussions seriously. If an athlete returns to play too soon after a concussion, the brain can suffer serious long-term consequences.
The American Academy of Pediatrics recommends that all student athletes in contact sports take baseline tests.
The estimates regarding the likelihood of an athlete in a contact sport experiencing a concussion may be as high as 19%, according to the Centers for Disease Control and Prevention. Data compiled from studies performed by Ohio State University College of Medicine show that perhaps 49% of high school athletes return to play too soon after a concussion.
- Signs and Symptoms of a Concussion
Signs Observed by Parents or Guardians
- Appears dazed or stunned
- Is confused about assignment or position
- Forgets an instruction
- Is unsure of game, score, or opponent
- Moves clumsily
- Answers questions slowly
- Loses consciousness (even briefly)
- Shows mood, behavior, or personality changes
- Can’t recall events prior to hit or fall
- Can’t recall events after hit or fall
Symptoms Reported by Athlete
- Headache or “pressure” in head
- Nausea or vomiting
- Balance problems or dizziness
- Double or blurry vision
- Sensitivity to light or noise
- Feeling sluggish, hazy, foggy, or groggy
- Concentration or memory problems
- Confusion
- Just not “feeling right” or “feeling down”
This information is from Centers for Disease Control and Prevention.
- Concussion - What to Do
Keep your teen out of play.
If your teen has a concussion, her/his brain needs time to heal. Don’t let your teen return to play the day of the injury and until a health care professional, experienced in evaluating for concussion, says your teen is symptom-free and it’s OK to return to play. A repeat concussion that occurs before the brain recovers from the first—usually within a short period of time (hours, days, or weeks)—can slow recovery or increase the likelihood of having long-term problems. In rare cases, repeat concussions can result in edema (brain swelling), permanent brain damage, and even death.Seek medical attention right away.
A health care professional experienced in evaluating for concussion will be able to decide how serious the concussion is and when it is safe for your teen to return to sports.Teach your teen that it’s not smart to play with a concussion.
Rest is key after a concussion. Sometimes athletes wrongly believe that is shows strength and courage to play while injured. Discourage others from pressuring injured athletes to play. Don’t let your teen convince you that s/he’s “just fine.”Tell all of your teen’s coaches, athletic trainers, and the student’s school nurse about ANY concussion.
Coaches, athletic trainers, and school staff should know if your teen has ever had a concussion. Your teen may need to limit activities while s/he is recovering from a concussion. Your teen may need to limit activities while s/he is recovering from a concussion. Things such as studying, driving, working on a computer, playing video games, or exercising may cause concussion symptoms to reappear or get worse. Talk to your health care professional, as well as your teen’s coaches, athletic trainers, school nurse, and teachers. If needed, they can help adjust your teen’s school activities during her/his recovery.This information is from Centers for Disease Control and Prevention.
- Concussion Test
MHS’s Sports Medicine Program recommends that student athletes have a baseline test prior to the beginning of the season. The baseline evaluation offered by us is the same one used by the NFL. It measures and records the athlete’s balance, cognition, eye movement, and visual acuity functioning. This baseline data is used comparatively if the athlete sustains a head injury.
The pre-season baseline screening provides an objective baseline measurement of the athlete’s postural stability using the BioSway Clinical Test for Sensory Integration of Balance, which is a computerized balance assessment tool. If a student-athlete experiences a concussion during the season, MHS Rehabilitation can perform the ImPACT test, a post-injury screening to assist the physician in making the “return to play” decision.
Parents requesting a baseline test are required to sign a consent form. The test is not covered by private insurance, but is offered for a nominal fee. Payment is required at the time of the appointment. To schedule an appointment, call MHS Rehabilitation and Sports Medicine at (785) 263-6664.
- Post-Concussion ImPACT Test
Memorial’s Sports Medicine Program uses ImPACT to assess athletes after a concussion. ImPACT stands for Immediate Post-Concussion Assessment and Cognitive Testing.
The data gathered through baseline and post-injury testing provides health professionals an objective way to monitor the athlete’s recovery so that an evidence-based decision can be made to evaluate when he/she can safely return to sport or work.
The post-injury assessments can be repeated as often as needed to show progressive recovery.

Contact Us
Memorial Health System Rehabilitation and Sports Medicine
511 NE 10th Street
Abilene, KS 67410
Phone: (785) 263-6664
Hours: Monday – Friday, 8:00 a.m. to 4:30 p.m.
Dr. Todd Herrenbruck, Orthopedics
Visiting Specialist
Salina Ortho
523 S. Santa Fe Ave.
Salina KS 67401
Phone: (785) 823-2215
Dr. Todd Reilly, Orthopedics
Visiting Specialist
Salina Regional Orthopedic Clinic
520 S. Santa Fe Ave., Ste. 240
Salina KS 67401
www.salinaregionalorthopedicclinic.com
Phone: (785) 452-7366
